Blog
Thinking about consent
Perspectives on informed consent, healthcare technology, medico-legal risk, and clinical governance.
Why a hash chain makes consent records medico-legally defensible
A consent form is a claim. The hash chain in a GetConsent evidence pack is the proof. Here is how SHA-256 chaining works and why it matters when a claim is contested in court.

Comprehension is the standard, not signature
Australian courts have been clear for decades: a patient can sign a form and still not have given informed consent. What the law actually requires, and what GetConsent is built to document.

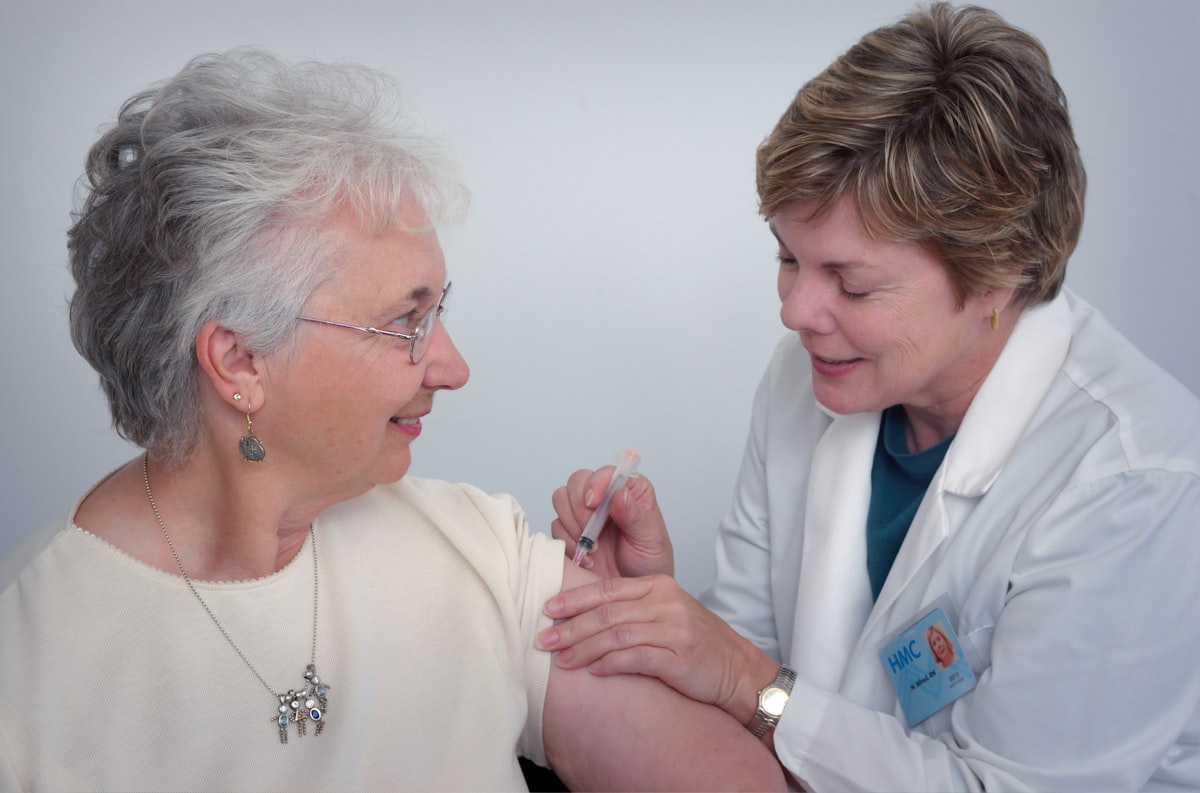
Building a consent form that works for every patient
Consent forms optimised for a 55-year-old English-speaking professional are not accessible consent. Audio read-aloud, 12 languages, WCAG 2.1 AA, and why we built all of it before launch.

AI-generated consent templates: where the AI stops and the clinician starts
We use AI to draft templates and translate them into 12 languages. We do not let AI publish them. Here is how the governance workflow works and why the distinction matters.
FHIR R4 Consent resources and what they mean for practice integration
FHIR R4 defines a Consent resource that maps almost exactly to the GetConsent evidence pack structure. How we handle compliance, and what it means for EMR integration.
Substitute decision-maker consent: what the platform needs to capture
When a patient cannot give consent themselves, the legal requirements multiply. Guardian name, relationship, legal basis, and capacity assessment: all must be in the record. How we handle it.